- Home
- Intolerances and Special Diets
- Gluten and Casein
How and Why to be On a Gluten and Casein Free Diet
Do you suspect you might need a gluten and casein free diet? Here's how to figure it out and how to make it work.
Pin For Later
You’ve been on a gluten free diet for a while now but things aren’t much better.
You still feel bloated much of the time and the bathroom situation is, well, messy…still. Are you frustrated? Of course you are, but you are not alone.
About 30% of people with celiac disease find their symptoms do not get better when they cut out gluten1. What then could be the problem?
First consider cross-contamination. Is it possible that you are still getting gluten from somewhere? Crumbs on the counter? Someone double dipping into your peanut butter?
If you’re pretty sure you’re not getting gluten, then you need to look for another cause. People with celiac disease often suffer from other food intolerances, and the most common is dairy.
Skip right to the section that interests you or read through to learn all about gluten and casein
What is Casein?
Casein is a protein in milk.
Milk, like all foods, can be broken down into it's three macro-nutrients: carbohydrate, protein and fat.
Lactose, which is the sugar in milk comes under the carbohydrate category. Casein is one of the many proteins in milk. It's the part of the milk that curdles to make cheese. The other main protein in milk is whey.
Both of casein and whey can cause allergies or intolerances, but the more common one is casein.
Why is Casein a Problem?
There may be a couple of things going on. First of all, not all casein is created equal and there are a few varieties that may not be well tolerated by humans.
The main one is alpha S1 casein2 which is most prevalent in bovine (cows) milk. Milk from other mammals have casein too but they have lower percentages of alpha S1.
Who Is Most Often Casein Intolerant?
People with celiac disease often have problems with casein. But casein allergy or intolerance is a condition all on its own, unrelated to celiac disease.
Up to 3 percent of children under the age of three have issues with cows milk3. This often surfaces in infancy as these children can’t digest formula made from cow’s milk. In these cases, if breast feeding is not an option, another formula like soy is usually the solution.
Some scientists think that even in these cases, casein intolerance may be a pre-cursor or even a trigger to celiac disease. Research is still ongoing.
Is Casein Gluten Free?
Yes, casein is gluten free and many people with celiac or gluten intolerance do just fine with casein or with dairy products in general.
Are There Similarities Between Gluten and Casein?
Both are proteins, and both seems to cause problems for a fair number of people. The reason why is still not well understood.
To explain casein intolerance in people with celiac disease, scientists have investigated “cross-reactivity” between gluten and casein. There is not a lot of research on this yet but it’s gaining some ground, so keep an eye. I certainly will and will provide updates as new info comes along.
Cross reactivity means that one substance “mimics” another in its effect on the immune system. With gluten and casein it may be that our immune systems somehow mistake the casein molecule for gluten and so we have a similar reaction.
Another example of a food protein that may be cross reactive to gluten is avenalin, from oats. That may be why so many people with celiac can’t tolerate even gluten free oats.
The chart below is from a laboratory study that shows cross reactivity of several different food proteins with α-gliadin or gluten. Gluten and casein is the most prevalent4.
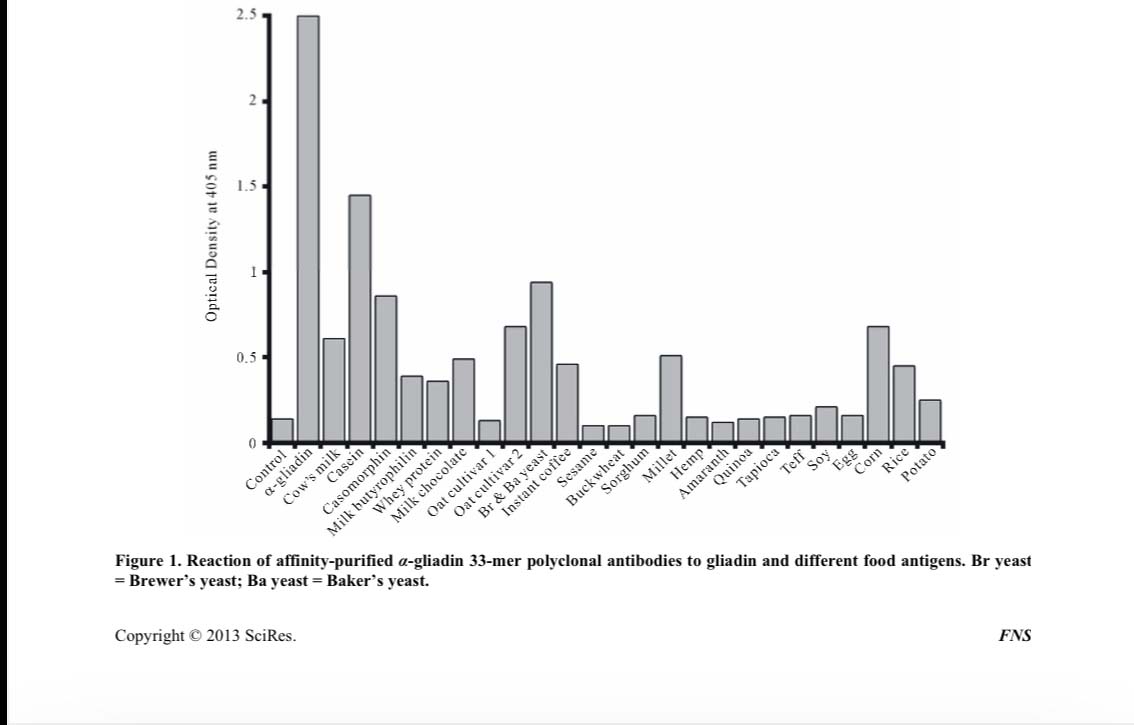
A Few Facts About Gluten and Casein:
If you like to geek out on this stuff like I do, here are some interesting facts:
- Baking “denatures” the protein so some people can tolerate milk in baked goods but not in raw or fluid form.
- Pasteurization does not heat the milk for long enough or at the right pH to denature the protein.
- Milk from different mammals have different casein profiles. This means some people who can’t tolerate cows milk are fine with goat, sheep or water buffalo milk.
- One study showed about 50% of celiac patients tested had a reaction to casein that was similar to gluten. This was compared to zero in the control group5. This seems to show a correlation between gluten and casein reactivity.
How Can I Tell if I'm I Intolerant to Lactose or Casein?
To find out if you are allergic to casein or another component of milk, you can go to an allergist and have a skin prick test.
For most folk who have problems with gluten and casein, the casein issue is more of an intolerance than an allergy and there is no test for that.
The only way to know if you have an intolerance to any food is to eliminate it from your diet and see if you feel better. If you cut out milk and find that your symptoms improve, then you’ve narrowed the problem down to dairy, that’s a start. To figure out if your issue is lactose or casein, you’ll need to look for a few more clues. I suggest first reading the article on lactose intolerance, then come back here. I’ll wait.
You just learned that many lactose intolerant people are okay with lactose free milk and ice cream, yogurt or hard cheeses. If you don’t tolerate these foods, then that’s a good clue that your issue is casein rather than lactose.
Another clue is if you have been gluten free for six months to a year and still can’t tolerate dairy products. Secondary lactose intolerance from celiac disease usually improves once the gut starts to heal.
Casein in Milk From Sheep, Goats and Other Mammals

Photo by Strvnge Films on Unsplash
All mammals produce milk for their young. It’s actually part of the definition of a mammal. We humans are the only mammal that drinks milk from other mammals and in North America, we drink mostly cows milk.
In some other parts of the world goat and sheep milk is more common, and that is making its way to North America, mostly in the form cheese. Water buffalo is another mammal who’s milk is made into cheese.
A1 Beta Casein vs A2 Beta Casein
Many people who cannot tolerate cows milk find that these other milks and cheeses are okay. Why is that?
The science is new on this so I couldn’t find a whole lot that is conclusive, but it seems to point to the difference between A1 beta casein, vs A2 beta casein. This kind of makes sense as cows milk is higher in the A1 variety and sheep, goat and water buffalo milk are lower in A1 and higher in A2.
This has caused some stir in the scientific community. It has even caused some groups to start to advocate for consumption of milk from certain breeds of cows that is higher in A2 beta casein. Beware however as the science is far from conclusive and there may be more marketing to this than fact.6
At the end of the day my best recommendation is to listen to your body. Try some alternatives and if they work for you then go with that. If not then you have your answer.
What to do if You Are Gluten and Casein Intolerant

As with gluten, the only way to deal with a casein intolerance is to avoid the source, in this case, dairy products.
Lucky for those of us who deal with this, there are a lot of options to substitute for dairy in your gluten free diet.
Plant based milks like coconut, almond, soy etc. are highly available and substitute just fine in cooking, baking and to pour on your cereal. Vegan "cheese" is also available and tastes pretty good. Of course it's a bit less "natural" so you need to decide if it's right for you.
If you're one of the lucky ones like me who can tolerate sheep and goat’s milk then your options are wider. The best thing about these alternative milks and cheeses, besides the taste, is the nutritional profile. You are still getting all of the nutrients from milk without the pain.
Does Goat and Sheep Cheese Have Casein?

Yes, but as you read above, goat and sheep milk are higher in A2 beta casein and lower in A1 beta casein which is more prevalent in cows milk. This is why a lot of people who can't tolerate cow's milk or cheese made from cows milk can have milk and cheeses from goats, sheep and even water buffalo.
 Zucchini lasagna made with goat cheese and vegan cheeses shreds.
Zucchini lasagna made with goat cheese and vegan cheeses shreds.Cheese made from these alternatives are great tasting, widely available and the variety is increasing all the time.
I love nice sharp goat cheddar on grilled cheese, or goat mozzarella on pizza ore lasagna. Soft goat cheeses come plain or garnished with herbs or cranberries. These make cheese sauces smooth and creamy or simply top off a gluten free cracker. Pecorino Romano from sheep’s milk is a lovely hard cheese that substitutes nicely for armesan.
Is Feta Cheese Okay for a Casein Free Diet?
True feta cheese is made from sheep or goats’ milk , so if you can tolerate these you may think you're good to go.
However, some feta cheese is made with cows milk so you need to check the label.
If you're ordering Greek salad in a restaurant or any other dish made with feta cheese be sure to ask if it's goat or sheep feta. Many restaurants will buy the cow's milk feta because it's cheaper.
Summary
- If your gluten free diet has not resolved all your symptoms, first look for cross contamination, then consider other food intolerances
- Dairy is the most common food intolerance that correlates with gluten. First consider lactose intolerance. If that's not it then it could be a gluten and casein cross-reactivity.
- The only way to treat a casein intolerance is to avoid cows milk.
- Milk from other mammals also has casein but some people can tolerate these. The only way to know is to try.
References
1. Vojdani, A., & Igal, T. (2013). Cross-Reaction between Gliadin and Different Food and Tissue Antigens. Food and Nutrition Sciences, 4, 20–23. https://www.scirp.org/pdf/fns_2013011516575568.pdf
2. Stout, J., MS. (2019, March 12). Is Goat Milk Gluten Free? Retrieved April 23, 2021, from https//mtcapra.com/is-goat-milk-gluten-free/
3. Demarco, P.,MD and Lupoli, T.,DO (2020). Milk Allergies: Understanding Milk Allergy Symptoms and Treatments. Retrieved April 23, 2021, from https://www.jaxallergy.com/allergy-treatments/food-allergies/milk-allergy/
4. Vojdani, A., & Igal, T. (2013). Cross-Reaction between Gliadin and Different Food and Tissue Antigens. Food and Nutrition Sciences, 4, 20–23. https://www.scirp.org/pdf/fns_2013011516575568.pdf
5. Vojdani, A., & Igal, T. (2013). Cross-Reaction between Gliadin and Different Food and Tissue Antigens. Food and Nutrition Sciences, 4, 20–23. https://www.scirp.org/pdf/fns_2013011516575568.pdf
6. Wikimedia Foundation. (2023, March 5). Casein. Wikipedia. Retrieved March 5, 2023, from https://en.wikipedia.org/wiki/Casein
Home > Intolerances and Special Diets
> Gluten and Casein















